
"Breast cancer is the most common cancer diagnosed among U.S. women (excluding skin cancers) with about 252,710 new cases expected to be diagnosed in 2017. [2,470 cases will be diagnosed in men. In addition,63,410 cases of in situ breast carcinoma will be diagnosed among women](2)
It is the second leading cause of cancer death among women in the U.S., after lung cancer; 40,610 women [480 men] in the U.S. are expected to die from this disease in 2017.
81% of breast cancers are diagnosed among women ages 50 years and older, and 89% of breast cancer deaths occur in this age group.
The median age at diagnosis for all women with breast cancer is 62 years; the median age at diagnosis is younger for black women than for white women; and the median age at breast cancer death is 68 years overall (70 years for white women and 62 years for black women)."(1)
The older a woman is, the more likely she is to get breast cancer.
Rates of breast cancer are low in women under 40. Fewer than 5 percent of women diagnosed with breast cancer in the U.S. are younger than 40.
Rates begin to increase after age 40 and are highest in women over age 70 (see Figure 2.1 below).
The older a man is, the more likely he is to get breast cancer. However, breast cancer is much less common in men than in women (see Figure 2.1 below).
The median age of diagnosis of breast cancer for men in the U.S. is 68.
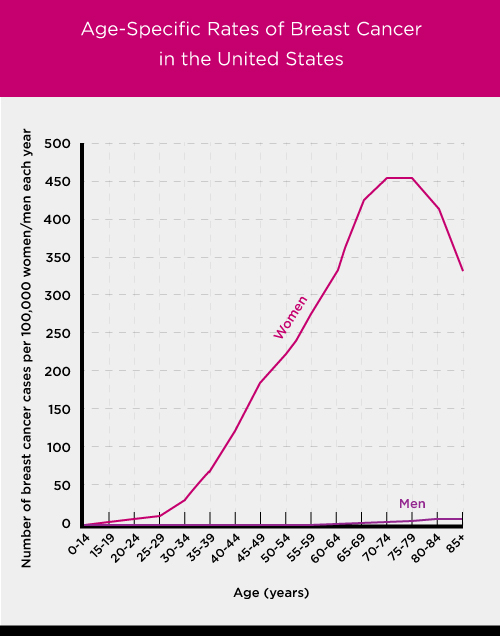
Data source: SEER 2011-2015 [2] Note: Though this graph shows a rate of 0 in some age groups, there are a few cases of breast cancer in these age groups. The numbers are too small, however, to appear on the scale used here.
Mammograms accurately diagnose Breast cancer in about 78 percent of all women tested, while diagnostic accuracy rises to about 83 percent for women over 50.(3)
Mammograms use radiation to make diagnostic decisions about performing a even more invasive procedure to "rule out" breast cancer. The radiation itself is a carcinogen.
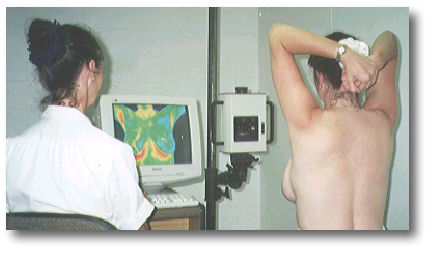
Thermograms DO NOT diagnose breast cancer, ever. They instead reveal "physiological" changes that suggest a change in the vascular system of the breast that may indicate a "problem" anywhere from hormone imbalances to an infection, a cyst or possibly a cancer. Further procedure(s) is/are necessary to DIAGNOSE what is going on.
Thus, Digital Infrared Thermal Imaging 'DITI' is a "adjunctive non-invasive test of physiology (or function)" that offers an increased opportunity of early detection. The screening is done without any pain, no radiation, or compression!
However, as you know, no breast test is 100% accurate. So it is important to consider a multimodal approach. Clinical trials have shown that Thermography significantly augments the long-term survival rates of its recipients by as much as 61%.(4) And when used as part of a multimodal approach (clinical examination, mammography, and infrared imaging) 95% of all early stage cancers will be detected.
A Thermogram is a test without any exposure to radiation that is used as part of an early detection program which gives women of all ages the opportunity to increase their chances of detecting breast disease at an early stage. It is particularly useful for women under 50 where mammography is less effective or in women with breast implants.
Dr. Schultz has been offering Thermography from NEWS for close to 20 years now. She likely has been offering this modality for the longest time span of any physician in the US. Why?.....Because she had too many women in the 1990's who did not want to radiate their breasts. Instead of offering them nothing, the "Thermogram with MediTherm" seemed safer than doing nothing at all.
While the 3D-Mammography of today is better for younger women with dense breasts, we still have the radiation to deal with. One day, in the near future, we will have a diagnostic blood test for that. For now, however, doing a baseline Mammogram in conjunction with a baseline Thermogram provides better assessment. After initial diagnostics and according to the risk assessment of the individual woman, it is suggested to repeat Thermograms every year a Mammogram is not done. Mammography guidelines recommend assessment every 1 to 2 years.
So what is a woman to do? Well let's remember how often opinions have changed over this very subject during the last 20-30 years.
In October 2015, the American Cancer Society (ACS) issued new recommendations that concluded that women at average risk of breast cancer start mammography at 45. ACS also advised women undergo annual mammograms from 45 – 54, and repeat mammography every other year after the age of 54.
Nothing is perfect; but a Self-Breast-Exam every month starting in your 20's, a Mammogram every 3 to 5 years from the ages of 40 to 75 [which is only 12 to 8 Mammograms], and Thermograms interspersed, seems a safer multi-modal option. While this is Dr. Schultz's personal plan, she takes into account your individual risks, and then advises a plan for you based on those risks at your consultation.
Our Thermography Partner is Mobile Thermographic Imaging (MTI) out of Atlanta, Georgia. They are MediTherm trained and belong to the ACCT American College of Clinical Thermology
They come to our office usually every other month and we ask that you call their office to schedule an appointment.
Mobile Thermographic Imaging Contact Information:
Main Office: 678-688-8986 | office@mobile-thermographic-imaging.com
Janique Cook, Co-Owner & Administration: 678-852-8548
Angelique Scibetta, Co-Owner & Accounting: 678-773-6563
Brandy Jackovitch, Office Manager: 404-790-3457
1. Breast Cancer Statistics, 2017 - American Cancer Society Press Room pressroom.cancer.org/BreastCancerStats2
2.
3. https://www.uchealth.org/today/2015/07/06/how-accurate-are-mammograms/
4. Gautherie, Ph.D.; Thermobiological Assessment of Benign and Malignant Breast Diseases. Am. J. Obstet. Gynecol., 1983; V 147, No. 8: 861-869.